Article
The FDA's Blood Donor Amendment for MSM is a Correction, not a Victory
Author(s):
Amid a blood shortage and continued stigmatization of HIV risk, it's hard to feel good about the FDA's delayed decision—though good may still come of it.
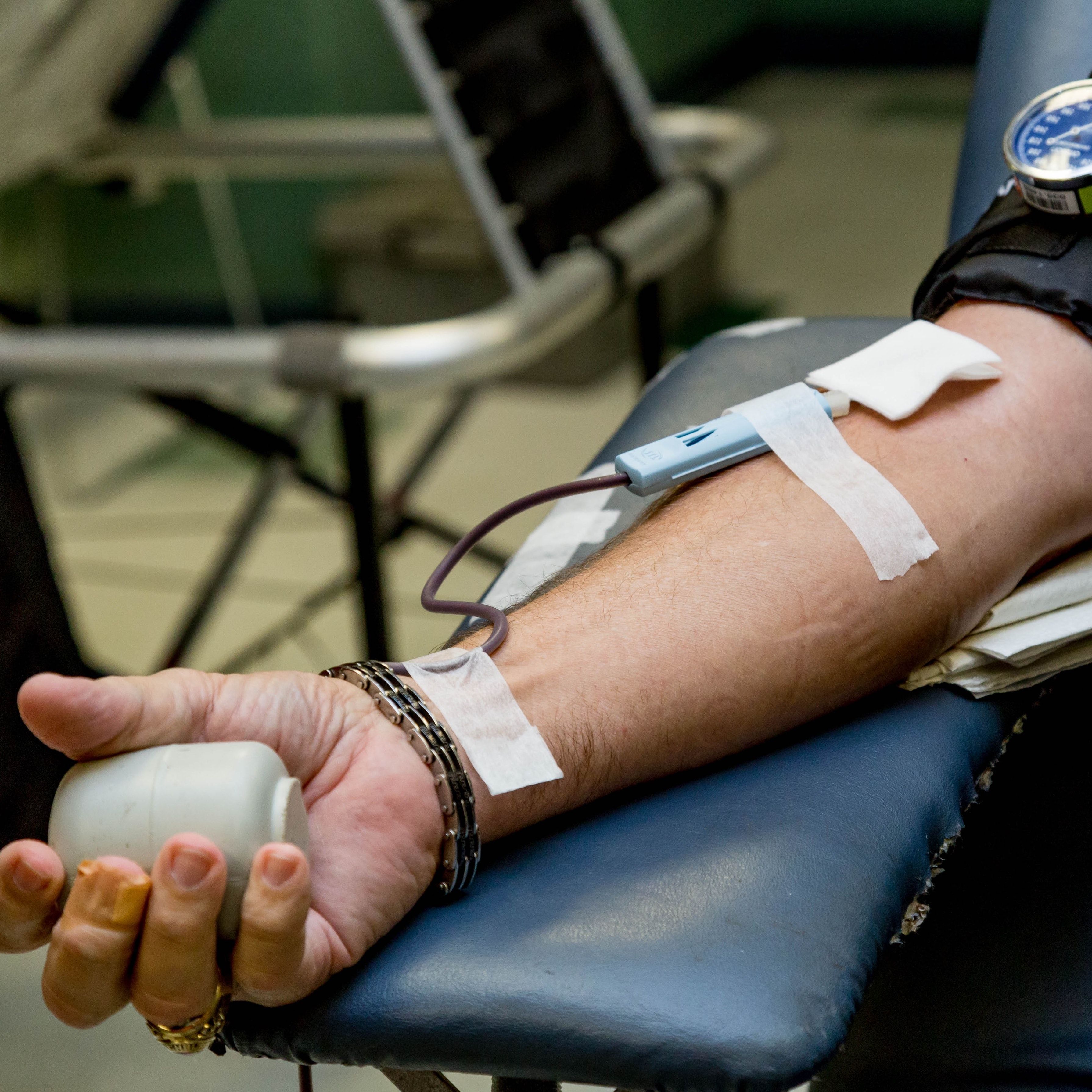
It is neither too little nor too late, though it somehow feels both.
Last week, the US Food and Drug Administration (FDA) issued a draft guidance amending the recommendations surrounding blood donor eligibility based on an individual’s risk of HIV transmission. In short, the FDA has altered guidance to eliminate the months-long deferral for men who have sex with men (MSM) and women who have sex with MSM in lieu of an “individual risk-based” questionnaire.1
The proposal makes no change to the current deferral time periods set for donors with other HIV risk factors including a history of exchanging sex for money or non-prescription injection drug use. It maintains that all blood establishments should continue to test blood donors for relevant infections including HIV and hepatitis B and C.1
Some other key notes regarding this alteration to MSM blood donor guidance: it is the latest correction to a standard set originally in April 1992—at a time when AIDS was the leading cause of death for all Americans aged 25 – 44 years old2—and it acknowledges the benefit and utility of pre-expsoure prophylaxis (PrEP), recommending that persons at risk of HIV taking PrEP be deferred anywhere from 3 months to 2 years based on their administration method and most recent dose.1
Consider some more context surrounding this decision being made, only now, in 2023:
- The FDA established the Transfusion Transmissible Infections Monitoring System (TTIMS) in 2015 to address risk of blood transfusion-related infections pertinent to these recommendations.3
- PrEP has been an available and efficacious preventive therapy for persons at risk of HIV in the US for more than a decade.
- Data from a 2014 literature review estimated that risk of HIV acquisition from sexual exposure were attenuated by 99.2% when antiretroviral therapy (ART) and condoms were used by the infected partner.4
- The US has been experiencing a blood donor crisis.
Indeed, the American Red Cross—supplier of approximately 40% of the nation’s blood—reported its “worst blood shortage in over a decade,” as their rate of blood donors had decreased 10% since the beginning of the COVID-19 pandemic.5 Local, regional and national blood banks have similarly reported shortages, as hospitals and emergency care facilities have had to make continually difficult decisions about the allocation of their blood and platelet supplies.
We’ve had outcome-altering HIV therapies and prophylaxes on the market for years. We’ve had blood-infection monitoring systems working on a national, real-time scale for years. We’ve been combating a vital resource shortage—during the greatest health crisis since the AIDS epidemic that first spurred these donor standards—for years. How is this proposal only being raised now?
Because proactivity is not prioritized in the US health care system. It would rather attempt to put out multiple blazes at once than invest in a fire alarm.
Consider the state of HIV in the US as it relates to relevant risks in our blood donor shortage. Though MSM accounted for approximately 71% of new HIV diagnoses nationally in 2020, annual cases among this population have been declining since 2016.6 What continues to challenge this population’s protection are access to testing and health literacy, a geographical shift in HIV cases, and continued stigma around HIV risk populations.
Once a coastal epidemic, HIV diagnoses have disproportionately affected the South for years now—constituting 12.4 cases per 100,000 people, or 51% of all US cases, in 2020, per the US Centers for Disease Control and Prevention (CDC).7 Among the 1.2 million estimated Americans with HIV, approximately 13% are unaware and require testing.6
HIV cases have been declining but also “migrating” toward regions with arguably greater historical burdens of discrimination against homosexuality, and lesser health literacy and resourcing. Couldn’t greater and earlier inclusion of high-risk populations like MSM in national blood donor drives have not only benefitted the shortage crisis, but improved the awareness of and access to HIV testing itself due to blood bank testing requirements?
Blood banks have had this secondary appeal embedded in its marketing for a couple years now; the Red Cross has continually promoted access to COVID-19 antibody results to its new and recurring donors since 2020 as part of its efforts to resolve the blood shortage.8 Americans are increasingly absent from health care settings, clinics and primary caregiver interactions during which time they would be privy to testing opportunities; a secondary outlet like a blood drive is a no-brainer opportunity to inform an individual of any other risks they may carry.
Whether the FDA’s proposal will be deemed a “win” by the MSM community remains exclusively their decision; many have gone their entire lives marginalized and mismanaged by our health care system due in part to archaic and fear-based responses to the HIV epidemic decades ago. Greg J. Zahner, MD, MSc, of Massachusetts General Hospital and Harvard Medical School, wrote in September 2020, “because I am gay, my blood is deemed too dangerous.”9
“The memory of the HIV/AIDS epidemic prior to current advances in testing and treatment, superimposed on the longstanding societal marginalization of homosexuality, has led to a policy that continues to exaggerate the risk of undetected HIV among many MSM,” Zahner wrote of the FDA’s donor guidelines.
It actually is too little, too late to prevent our blood shortage or fix the public health flaws of HIV prevention post-epidemic. But we still have time to combat both issues if we look at the FDA’s donor amendment as not mission accomplished, but a mutual step toward MSM inclusion and HIV screening promotion.
References
- FDA Proposes Individual Risk Assessment for Blood Donations, While Continuing to Safeguard U.S. Blood Supply. News Release. US Food and Drug Administration. January 27, 2023. Accessed February 5, 2023. https://www.fda.gov/news-events/press-announcements/fda-proposes-individual-risk-assessment-blood-donations-while-continuing-safeguard-us-blood-supply
- A Timeline of HIV and AIDS. HIV.gov. Accessed February 5, 2023. https://www.hiv.gov/hiv-basics/overview/history/hiv-and-aids-timeline#year-2022
- Williams A. TTIMS: Transfusion-Transmissible Infections Monitoring System: Program Overview. Blood Products Advisory Committee: March 21, 2019. Accessed February 5, 2023. https://www.fda.gov/media/127508/download
- Patel P, Borkowf CB, Brooks JT, Lasry A, Lansky A, Mermin J. Estimating per-act HIV transmission risk: a systematic review. AIDS. 2014;28(10):1509-1519. doi:10.1097/QAD.0000000000000298
- Red Cross Declares First-ever Blood Crisis amid Omicron Surge. News Release. American Red Cross. January 11, 2022. Accessed February 5, 2023. https://www.redcross.org/about-us/news-and-events/press-release/2022/blood-donors-needed-now-as-omicron-intensifies.html
- U.S. Statistics. HIV.gov. Accessed February 5, 2023. https://www.hiv.gov/hiv-basics/overview/data-and-trends/statistics
- Diagnoses of HIV infection in the United States and dependent areas, 2020. HIV Surveillance Report 2022;33. Accessed February 5, 2023. https://www.cdc.gov/hiv/library/reports/hiv-surveillance/vol-33/index.html
- Red Cross testing blood donations for COVID-19 antibodies. News Release. American Red Cross. March 10, 2022. Accessed February 5, 2023. https://www.redcrossblood.org/local-homepage/news/article/red-cross-testing-blood-donations-for-covid-19-antibodies
- Zahner GJ. We Need Blood and I Am Not Allowed to Help. JAMA Intern Med. 2020;180(12):1571–1572. doi:10.1001/jamainternmed.2020.4331





