Publication
Article
Family Practice Recertification
Newborn with Buttocks Lesion
Author(s):
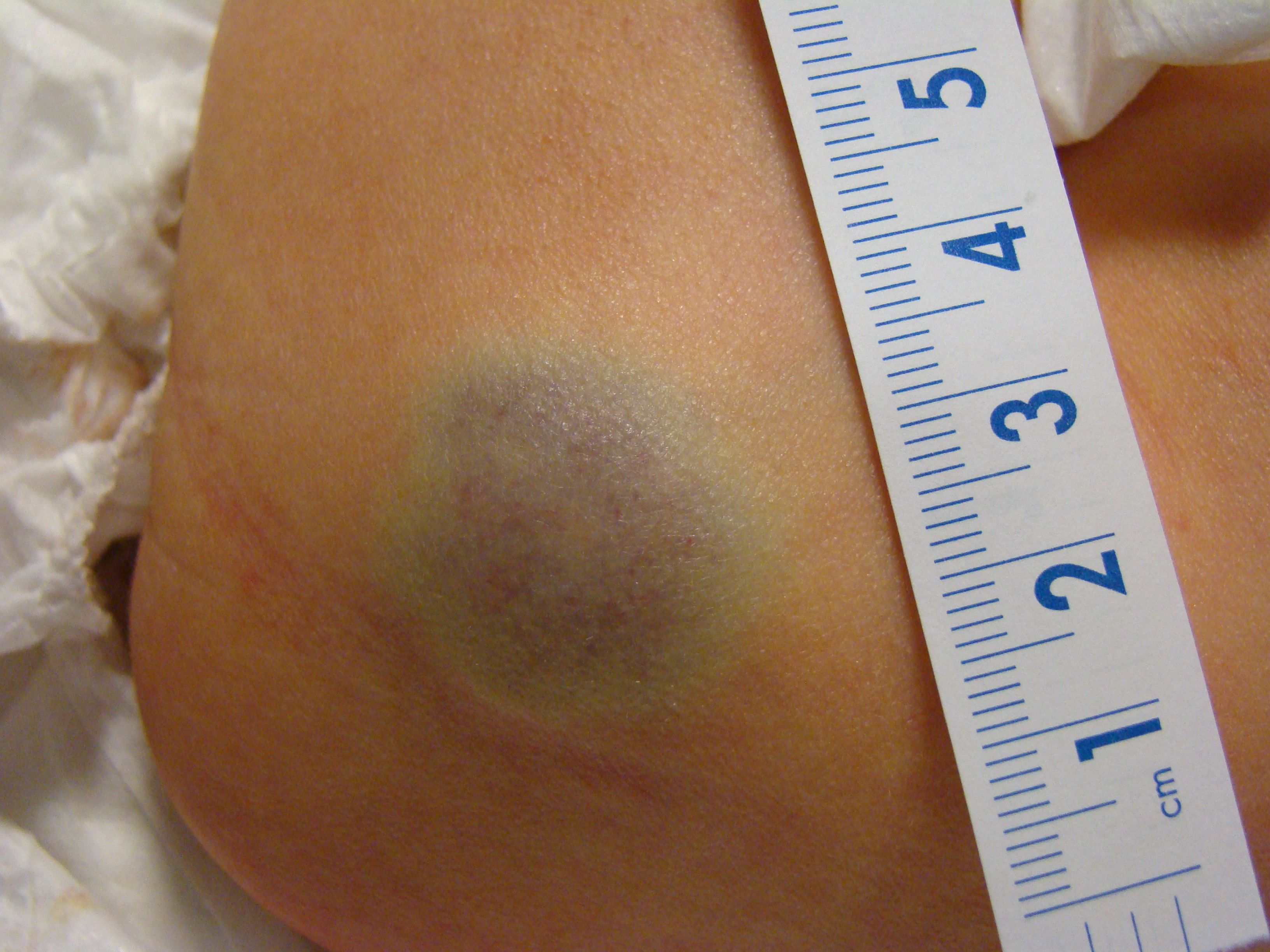
This 3-day-old boy was noted to have this left buttock lesion. He was born by cesarean section at 35 weeks due to a transverse lie on presentation with premature rupture of membranes. There was no prenatal care, and routine maternal labs on admission were significant for a positive gonorrhea screen.
This 3-day-old boy was noted to have this left buttock lesion. He was born by cesarean section at 35 weeks due to a transverse lie on presentation with premature rupture of membranes. There was no prenatal care, and routine maternal labs on admission were significant for a positive gonorrhea screen.
What is your diagnosis?
- Deep hemangioma
- Blueberry muffin syndrome
- Congenital blue nevus
- Gonorrhea
- Ecchymosis
Diagnosis
This deep hemangioma is one type of infantile hemangiomas that range from superficial “strawberry hemangiomas,” to even larger deep hemangiomas that can involve viscera and underlying structures. Infantile hemangiomas will usually grow, often rapidly, during the first year of life and then gradually involute, reducing in size over the next 5 to 7 years. Small lesions and those in unobtrusive areas like this infant’s lesion do not require any treatment.
Large lesions and those that compress adjacent structures, especially on the face causing dysfunction, usually respond well to propranolol. Occasionally lesions will rebound after the propranolol is stopped, but usually respond to a repeat course. Oral prednisone was the previous drug of choice and these lesions can also be treated with injected steroids or laser.1
Blueberry muffin syndrome is the result of congenital rubella infection. It causes multiple violations of the skin-- lesions ranging from small flat lesions (macules) to raised plaques in contrast to this infant’s single large lesion. Maternal infection prior to 18 weeks is associated with a very high risk of congenital anomalies including intellectual disability, heart defects, loss of hearing and loss of vision.2
Congenital blue nevi are due to a localized proliferation of melanocytes. Their color is due to increased melanin in the melanocytes and associated macrophages. In contrast, the blue color in this child's lesion is due to increased vascularity.3
Gonorrhea can lead to infections in the neonatal, but most commonly presents with conjunctivitis. It is usually passed vertically to the infant during vaginal delivery or with ruptured membranes, so the infant would not be born with such findings.4
Ecchymosis is common in vaginal deliveries but usually on the presenting part of the infant, especially if there is a face presentation. It usually presents in a more diffuse pattern and would fade with time as opposed to increasing in size like a deep hemangioma tends to do.
References
[1] Shehata N, Powell J, Dubois J, Hatami A, Rousseau E, Ondrejchak S, McCuaig C. Late rebound of infantile hemangioma after cessation of oral propranolol. PediatrDermatol. 2013 Sep-Oct;30(5):587-91.
lesions and extensive metaphysitis. J Clin Diagn Res. 2014 Dec;8(12):PD03-4.
[2] Ajij M, Nangia S, Dubey BS. Congenital rubella syndrome with blueberry muffin
highlighting atypical and newly described variants, distinguishing features and
diagnostic pitfalls. Adv Anat Pathol. 2009 Nov;16(6):365-82.
[3] Murali R, McCarthy SW, Scolyer RA. Blue nevi and related lesions: a review
Perinat Neonatal Nurs. 2000 Jun;14(1):17-38.
[4] Mancuso P. Dermatologic manifestations of infectious diseases in pregnancy. J
About the Author

Daniel Stulberg, MD, is a Professor of Family and Community Medicine at the University of New Mexico. After completing his training at the University of Michigan, he worked in private practice in rural Arizona before moving into full-time teaching. Stulberg has published multiple articles and presented at many national conferences regarding skin care and treatment. He continues to practice the full spectrum of family medicine with an emphasis on dermatology and procedures.






